off the charts
POLICY INSIGHT
BEYOND THE NUMBERS
BEYOND THE NUMBERS
The Growing State Cost of Not Expanding Medicaid
Receive the latest news and reports from the Center
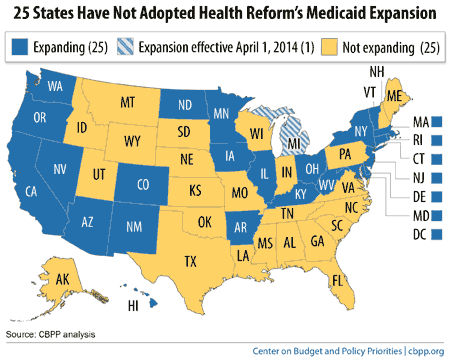
Policymakers in some of the 25 states that haven’t expanded Medicaid as part of health reform (see map) are putting expansion at the top of this year’s legislative agenda. The New Hampshire House passed an expansion bill on the first day of its session last week, for example, and Virginia Governor Terry McAuliffe advocated for expansion in his first address to lawmakers. These policymakers are wise to prioritize the Medicaid expansion, as the costs of not expanding have begun to accrue: